Sean Anderson
Hearing scientist and statistician.
Code on Github at seanranderson Hosted on GitHub Pages — Theme by mattgraham
Caveat: These views are my own and have not been endorsed or approved by anyone, including my employer.
Overview
I study how the two ears work together to figure out where sounds are located and understand speech in background noise. These make up binaural or spatial hearing. It is easy for people with typically developed hearing to take this for granted. However, much research shows that there are benefits of providing access to sound in both ears for people who experience hearing loss (see this paper for a review of clinical guidelines). For this reason, providing hearing to both ears is becoming the standard of care in audiology.
I have been working with people who experience hearing loss to study the benefits and limitations of spatial hearing since 2013. My undergraduate and doctoral research focused on patients who have cochlear implants, and my post-doctoral research focuses on hearing loss that is difficult to diagnose using traditional techniques. The purpose of this page is to give a small overview of what we think happens for people who experience hearing loss that interferes with their ability to gain the benefits of spatial hearing. My mentors, peers, mentees, and I have worked with this framework to come up with solutions for how to improve outcomes for patients by advancing means of clinical assessment and improving hearing devices.
Locating Sounds
Sound source localization is the process by which people identify where sounds are located around them. The classic way to study this is to present sounds from speakers around someone’s head and ask them where the sound came from. Alternatively, researchers can manipulate sounds presented over headphones to provide cues suggesting that the sound was presented from a particular location (called “virtual acoustic space”). My and others’ research has shown the following patterns related to patients who experience hearing loss compared to age-matched, typically hearing peers:
- Poorer resolution of sound source localization
- Poorer sensitivity to the cues used to localize sounds
- Poorest outcomes for older listeners with hearing loss
- More variable outcomes across individuals, with some people performing quite well and others very poorly
If we think of the auditory system as applying a spotlight-like filter to the environment, then accurate localization performance occurs when the the spotlight is narrow (shown on the left below). On the other hand, when localization is poor, the spotlight is wide, resulting in more frequent and greater errors (shown on the right below).
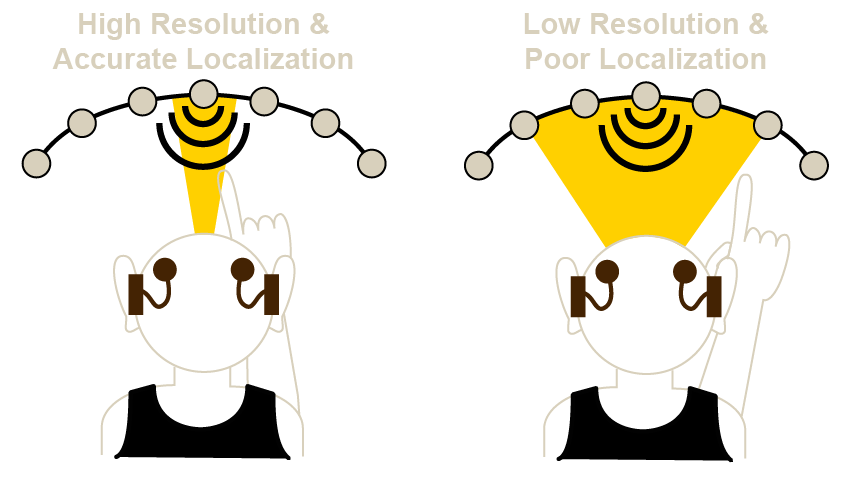
The questions many of us try to answer are: Why? What factors contribute to poorer performance and how do we diagnose and address them? In contrast to a lot of other neuroscience research, the auditory system has some well-defined neural circuits that seem to be involved with locating sounds. My research has focused on one particular circuit, the lateral superior olive.
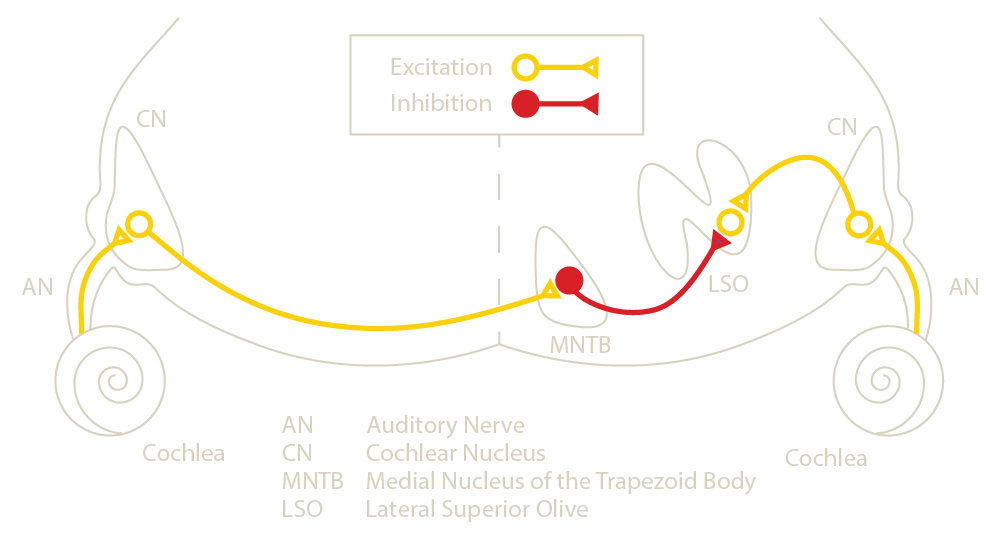
The lateral superior olive sits near the middle of the brainstem and responds to changes in the location (left vs. right) of high-frequency and short sounds. Specifically, the lateral superior olive seems to respond to the difference between the time of arrival and intensity of the sound in each ear. These are referred to as interaural time differences (ITDs) and interaural level differences (ILDs). I study the lateral superior olive by measuring electrical responses using minimally invasive methods and modeling its responses using computer programs.
Telling Sounds Apart
Sound source segregation is the process by which the auditory system separates one sound from another. Because this is so general, there is no “classic” way to address this problem. Different researchers have used sounds as simple as sine tones or as complicated as mixtures of speech. My and others’ research has shown the following patterns for patients who experience hearing loss compared to age-matched, typically hearing peers:
- Poorer speech understanding with background noise
- Greater effort to understand speech in noise
- Poorer ability to determine when one versus multiple sounds are presented
- Poorer sensitivity to cues that are used to distinguish between sounds
- More variable outcomes across individuals, with some people performing quite well and others very poorly
Instead of hearing two sounds as separate and coming from different locations (shown on the left below), it is suspected that listeners with hearing loss may fail to segregate sounds and instead link them together (“fuse” them; shown on the right below). This makes it more difficult to determine additional information about a sound (e.g., what word was spoken).

For the most part, studies have focused on sound source segregation or the percentage of correctly understood words, not both. Only recently have studies begun addressing both simultaneously.
My Work and Future Directions
Researchers have developed an extensive understanding of how spatial hearing works in the typically developed auditory system using many creative approaches. This is a difficult problem and efforts have taken place over centuries. More recently, the focus has shifted to improving the lives of patients who experience hearing loss. Accordingly, many new factors need to be considered, like:
- What differences are there in the neural circuitry from the typically developing system?
- How does hearing loss interact with other factors, like older age, to affect patients?
- What impact do different hearing devices, like hearing aids and cochlear implants, have on perception and auditory neural responses?
One factor that I have explored in my research is differences between the ears within the same patient. In other fields, like cognitive science for example, it is taken as a given that one side of the brain may be more efficient at processing certain kinds of information. Spatial hearing research on the other hand usually assumes that the ears of individuals are similar to one another. However, there is increasing evidence that patients who experience hearing loss tend to have a “better ear” (e.g., better hearing thresholds or speech understanding), and this is not considered in most clinical interventions. In fact, hearing devices may introduce greater differences between the ears, leading to poorer outcomes.
In my and others’ work, a few consistent trends have been found:
- Two ears are better than one, even if the second ear is difficult to understand.
- Spatial hearing outcomes (e.g., sound source localization and speech-in-noise understanding) may be limited by the worse ear.
- It is difficult to ignore the better ear, regardless of whether it is on the left or right side.
- It may be difficult to perceive clear and coherent sounds, especially when the ears are very different. Instead, listeners may perceive one amorphous sound when multiple sound sources are present, or multiple sounds when one sound source is present.
This research is still very new, and much needs to be done to determine how to use this new information to help patients. Because restoring hearing in both ears is associated with better outcomes than restoring hearing in only one ear, our focus has mainly been to determine how to promote the best spatial hearing outcomes and identify how to prevent major differences between the ears from developing for patients. Some promising results show that training patients to localize sounds or understand speech, giving a person access to hearing as early as possible, and matching devices across ears lead to better outcomes.
I plan to continue to dedicate myself to studying and addressing differences in hearing outcomes between the ears as long as I am doing hearing research. I hope to work with people who may be especially at risk of experiencing asymmetric hearing loss and collaborate on realistic and effective interventions. I plan to use my position and power to contribute to the advancement of students and researchers who are traditionally underrepresented in hearing science, including but not limited to Black, Indigenous, and all other people of color; people who identify as transgender or cis-gender female; people with disabilities, including hearing loss; members of the LGBTQ+ community; economically disadvantaged and first-generation students.
Dissertation
If you would like to read an extensive collection of my original research, my doctoral dissertation is available for free online from the University of Wisconsin-Madison. Each chapter is currently being prepared and submitted for publication in academic journals.
Publications
If you would like to read a copy of one of these publications and are unable to access it, please reach out to me via the Contact form on this website and I would be happy to provide it to you.
Grants
Anderson, S. R. (2020). Mechanisms that underlie poorer binaural outcomes in patients with asymmetrical hearing and bilateral cochlear implants. National Institute on Deafness and Other Communication Disorders, F31 DC018483-01A1.